Key Takeaways
- Know the Risks: Infection, implant failure, peri-implantitis, and mechanical issues can occur but are manageable.
- Patient Factors Matter: Smoking, poor oral hygiene, systemic conditions, and a history of gum disease increase the risk of complications.
- Assess Before Surgery: Medical history, oral exams, imaging, and patient education reduce risks.
- Prevent and Monitor: Hygiene, disease management, follow-ups, and modern tools improve outcomes.
- Proactive Care: Combining prevention, education, and technology ensures safer, long-lasting implants.
Introduction
Implant procedures stand at the forefront of modern medicine and dentistry, offering transformative outcomes for patients seeking to restore function, aesthetics, and quality of life. While implant technology continues to improve, ensuring positive outcomes relies heavily on a full understanding of inherent risks and reductions in complications through evidence-based protocols, multidisciplinary care, and ongoing patient engagement. The ever-evolving standards at the Pikos Institute exemplify the commitment required to optimize patient outcomes across a range of implant procedures.
With the right risk mitigation strategies, most complications can be prevented or effectively managed. This not only ensures the health and safety of each patient but also prolongs the implant’s functional lifespan. A comprehensive approach includes recognizing procedure-specific risks, tailoring care to individual needs, and using both conventional and advanced assessment tools to anticipate and respond to issues before they escalate. The ultimate goal is to harmonize patient experience, safety, and satisfaction throughout the implant journey.
Common Risks Associated with Implant Procedures
Implants have an excellent safety record, yet certain complications remain possible. Among the most frequently encountered risks:
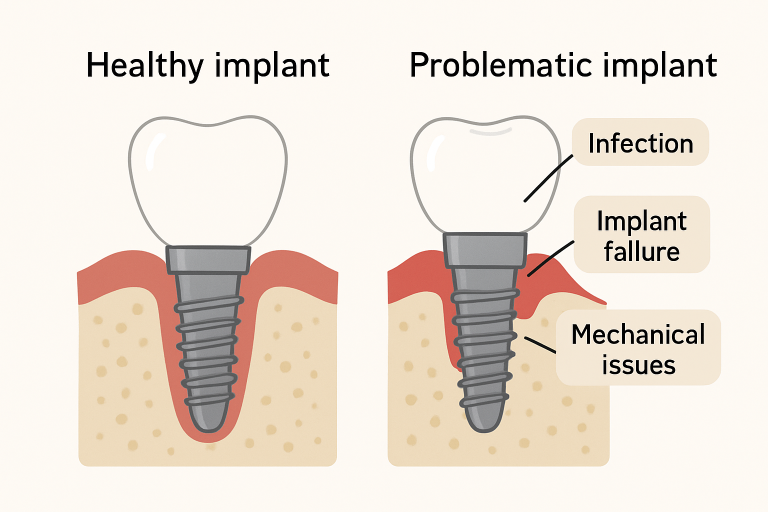
- Infection: Despite sterile protocols, infections can occur and may jeopardize implant integration or even require removal if not addressed swiftly.
- Implant Failure: Whether due to insufficient bone support, poor healing, or biomechanical overload, implants can fail to fuse to the bone effectively (a process called osseointegration).
- Peri-Implantitis: This inflammatory reaction affects the tissues surrounding the implant and can lead to bone loss if left untreated. It has symptoms similar to gum disease but requires specific intervention.
- Mechanical Complications: Problems such as implant fractures, screw loosening, or prosthetic component wear can undermine long-term results.
Identifying Patient-Specific Risk Factors
Personalized risk profiles are critical to guiding care and predicting potential complications. Some of the most important patient-specific risk factors include:
- Smoking: Smokers experience higher rates of complications due to impaired tissue healing and increased vulnerability to infection.
- Poor Oral Hygiene: Insufficient cleaning and maintenance can allow bacterial colonization, increasing the risk for infections such as peri-implantitis.
- Systemic Conditions: Medical issues like uncontrolled diabetes, autoimmune disorders, or osteoporosis can negatively impact bone healing and immune response.
- History of Periodontal Disease: Patients who have previously been treated for gum disease are more likely to experience issues around the implant site.
Pre-Operative Risk Assessment Strategies
The foundation of successful implant therapy is a careful, holistic evaluation before surgery. Essential steps include:
- Comprehensive Medical History: Reviewing conditions, medications, allergies, and previous surgical outcomes provides crucial context.
- Oral Examination: Assessing soft tissues, bone structure, and periodontal health to spot potential complications.
- Radiographic Imaging: Using X-rays or three-dimensional imaging technologies to determine the quality and quantity of available bone.
- Patient Education: Discussing realistic outcomes, procedural steps, risks, benefits, and aftercare requirements fosters trust and commitment.
Implementing Preventive Measures
With targeted prevention, many risks can be reduced or avoided entirely. Effective preventive strategies involve:
- Smoking Cessation Programs: Supporting patients to quit or reduce smoking significantly improves healing potential.
- Oral Hygiene Instruction: Providing clear, actionable guidance on brushing, flossing, and the use of adjunctive cleaning tools is vital for long-term success.
- Systemic Disease Management: Coordination with the patient’s physician to control underlying health conditions (such as diabetes) helps ensure a safer procedural outcome.
- Antibiotic Prophylaxis: In some cases, antibiotics are recommended to prevent infections, particularly for patients with elevated risk factors.
Monitoring and Managing Post-Operative Complications
After the procedure, proactive monitoring is essential for early detection and intervention if complications arise:
- Regular Follow-Ups: Scheduled evaluations allow for ongoing assessment of tissue healing and integration.
- Professional Cleanings: Consistent dental hygiene appointments are instrumental in maintaining implant and overall oral health.
- Patient Education: Reinforcing maintenance routines, warning signs of infection, and reasons for prompt care increases patient empowerment and participation in their treatment plan.
Advancements in Risk Assessment Tools
Modern technology is transforming the prediction and management of implant risk. Notable advancements include:
- Ultrasonic Elastography: This innovative tool detects subtle changes in implant stiffness over time, providing early alerts for structural fatigue or micro-movements, enabling timely clinical responses.
- Electronic Health Records (EHR) Analysis: Machine learning models analyze large datasets to identify trends and early warning signals in implant outcomes, thereby personalizing surveillance and optimizing interventions.
Final Thoughts
Optimal outcomes in implant procedures rely on addressing risks before, during, and after surgery. By employing comprehensive assessments, patient-focused education, and advanced monitoring technologies, care providers strengthen both short-term results and long-term implant viability. Embracing a proactive, evidence-based approach ensures patient safety and the enduring success of every implant.
MOBI ROLLER is a tech enthusiast with a background in technology. He writes about the latest trends, tools, and innovations in the tech world, sharing insights based on both knowledge and experience.

