Key Takeaways
- Artificial intelligence (AI) is improving early detection and enabling more precise, personalized spinal care.
- Minimally invasive techniques are setting new standards for spinal procedures, leading to faster recovery and better outcomes.
- Collaborative care models are central to effective, patient-centered prevention and management of spinal health.
Table of Contents
- AI in Spinal Health
- Minimally Invasive Techniques
- Collaborative Care Models
- Future Directions
Maintaining spinal health is increasingly recognized as a foundation for long-term well-being. As understanding of the spine’s role in whole-body wellness has grown, so have options for proactive care. Today, rapid advances in technology and interdisciplinary collaboration are giving rise to more dynamic preventive strategies, including highly tailored solutions like chiropractic care and sophisticated digital monitoring. These developments are helping to prevent injuries and chronic conditions before they take hold, transforming the patient experience from reactive to proactive. With back pain and spinal dysfunction impacting millions each year, preventing issues before they become debilitating is crucial. Innovations span artificial intelligence, minimally invasive surgical techniques, and comprehensive team-based care models. Together, these changes reflect a broader commitment among healthcare professionals to intervene earlier and support the spine throughout all stages of life. The result is a growing expectation that spinal care can not only resolve pain, but also extend quality of life and reduce healthcare costs.
AI in Spinal Health
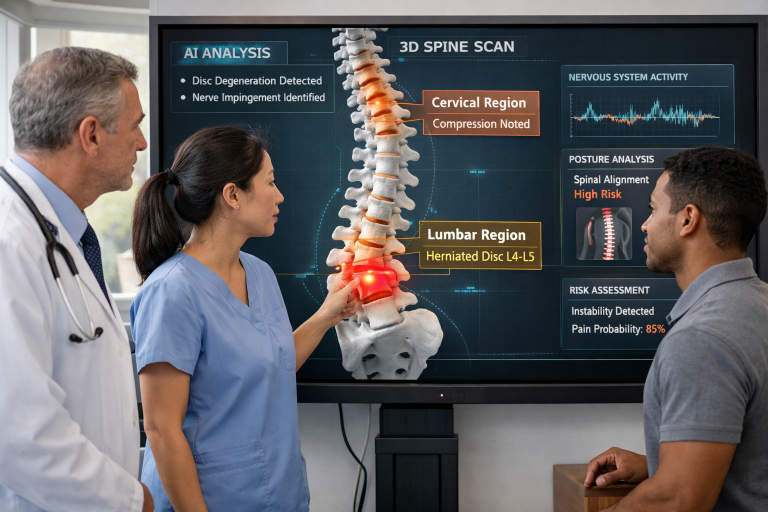
The emergence of artificial intelligence in spinal healthcare is influencing how providers detect and address musculoskeletal problems. AI-driven tools can rapidly review imaging and medical records to highlight patterns and early markers of spinal degeneration that can go unnoticed during routine screenings. By harnessing large datasets and recognizing subtle anomalies, these systems empower clinicians to identify risks before symptoms become severe or irreversible.
Personalization is another major advantage. AI can help design individualized prevention and rehabilitation plans by analyzing lifestyle, activity levels, genetic markers, and prior treatment data. This means that patients receive recommendations tailored not only to their spinal condition, but also to their unique body mechanics and risk factors. The potential to quickly adapt prevention strategies as a patient’s needs change could prove game-changing for long-term spinal health management. In addition, AI technology continues to play a vital role in the education of both patients and professionals. With machine learning–powered platforms, detailed visualizations, and predictive simulations, patients can now understand their condition and the effects interventions may have over time. Meanwhile, clinicians gain insights from aggregated data trends and predictive modeling that inform their recommendations, potentially identifying risk factors specific to certain populations that might not be apparent through traditional means. Over time, this integration of advanced analytics stands to substantially improve outcomes and raise the standard of spinal health care for diverse patient groups worldwide.
Minimally Invasive Techniques
The field of spine surgery has shifted dramatically with the development and refinement of minimally invasive approaches. Procedures such as endoscopic spine surgery, laser interventions, and percutaneous instrumentation allow for surgical correction with dramatically smaller incisions than standard open surgery. This often results in less tissue damage, shorter hospital stays, and reduced risk of infection or other complications.
For many individuals, this means that effective surgical intervention is accessible earlier and with less concern about lengthy rehabilitation periods. For example, endoscopic decompression of herniated discs or stenosis now routinely lets patients return to daily activities much faster than in the past. According to the Mayo Clinic, minimally invasive spine surgery continues to evolve, with outcomes for select conditions now rivaling or surpassing those of traditional surgery. Newer advancements in spinal implant technology, such as bioactive materials and customized 3D-printed devices, also have the potential to revolutionize recovery and restoration of spinal function. These tailor-made solutions promote better fusion, enhance compatibility with the patient’s anatomy, and reduce the risk of rejection or complications. Non-surgical techniques, such as regenerative medicine using stem cells and biologics, further complement minimally invasive interventions, potentially enhancing the body’s natural healing processes and preventing the escalation of degenerative conditions.
Collaborative Care Models
Prevention and management of spinal health issues are most effective when tackled by a diverse team. Collaborative care brings together physicians, physical therapists, chiropractors, occupational therapists, and other specialists in an integrated approach. By focusing on the whole patient instead of just the immediate problem, these teams can develop long-term strategies for spinal wellness. This patient-centered approach not only encourages early intervention and continuity of care but also supports education on posture, body mechanics, and lifestyle changes to prevent injuries. Many collaborative care models emphasize proactive screening and counseling, ensuring that issues are addressed before they lead to chronic dysfunction. As the Harvard Health Blog notes, multidisciplinary care has proven effective for individuals with complex spinal issues that are otherwise difficult to manage. Integrated care is becoming increasingly accessible as digital health platforms become more widespread. Secure messaging, remote consultations, and wearables that track mobility or discomfort levels keep the care team connected and allow providers to respond promptly when a patient’s status changes. By fostering regular communication and collaboration, modern care teams can better track progress, modify interventions quickly, and deliver holistic support that addresses not only the initial spinal complaint but also underlying risk factors.
Future Directions
The next decade promises even more exciting advances as these innovations converge. Artificial intelligence will continue to become more sophisticated, enabling patients and providers to access real-time risk assessment and progress tracking. Minimally invasive options will expand, enabling preventive procedures and regenerative therapies that promote healing at the earliest stages of injury or degeneration.
Furthermore, the trend toward collaborative care is likely to grow, with digital communication tools and telemedicine making it easier than ever for specialists to coordinate care. Incorporating preventive spinal care into primary health checkups and routine screenings may soon become the norm as awareness of spinal health’s impact on overall quality of life grows. By embracing these changes, patients and clinicians alike can look forward to a future in which spinal problems are detected early, treated gently, and managed holistically and long-term. As public health campaigns and educational outreach increasingly emphasize the value of spine health, communities will also benefit from greater access to evidence-based prevention programs. Schools, workplaces, and community centers may soon collaborate more closely with healthcare organizations to promote physical activity, ergonomic education, and early screening for spinal issues, ultimately reducing the prevalence and severity of musculoskeletal problems. Through shared commitment and ongoing innovation, the landscape of preventive spinal healthcare is poised to continue evolving, ensuring better health outcomes for current and future generations.
Conclusion
The future of spinal care is being reshaped by technology, minimally invasive techniques, and team-based approaches. Artificial intelligence enhances early detection and enables highly personalized treatment plans, while minimally invasive procedures reduce recovery time and improve outcomes. Collaborative care models ensure that prevention and management are patient-centered, addressing both immediate symptoms and long-term wellness. By integrating these innovations, spinal healthcare is shifting from reactive treatment to proactive prevention, offering patients faster recovery, better quality of life, and more informed, holistic care. Embracing these advances empowers both clinicians and patients to achieve stronger, healthier spines over a lifetime.
MOBI ROLLER is a tech enthusiast with a background in technology. He writes about the latest trends, tools, and innovations in the tech world, sharing insights based on both knowledge and experience.

